There are two families of ticks, the Ixodidae (hard ticks) and Argasidae (soft ticks). Those of importance to hikers, campers, and pet owners are in the family Ixodidae. Therefore, this publication covers species of that group. Several species are important because they bite people and/or pets.
Some can also transmit diseases to the people or pets they bite.
This publication will help you learn what ticks look like, how they live, the diseases they spread, how to manage tick problems, and how to protect yourself from tick-borne diseases.
New Hampshire Tick Species
The American dog tick, Dermacentor variabilis, is the most frequently encountered tick in New Hampshire. It is about 1/8” (4-5mm) long, brown and tan, with an obvious mottled pattern of surface markings on the back (opposite the belly side). It is a “threehost tick,” so named because it must find and feed on an animal three times to complete its two- year life cycle. This species has now spread to every county in the state. Parts of Cheshire, Sullivan, Grafton and northern Coos don’t have many.
The dog tick begins life as an egg, one of hundreds laid in a mass on the ground by a female tick. The egg hatches into a larva, which has six legs. The larva remains on the ground in leaf litter, or in low vegetation while waiting for a small mammal (usually a rodent) to brush by. It attaches to the animal and feeds for several days. Then it drops off and molts to the nymph stage, which has eight legs. Again it waits for a host (usually a rodent) to brush by. When that happens, the tick attaches and feeds on it for several days. When fully fed it drops off and molts to the adult stage.
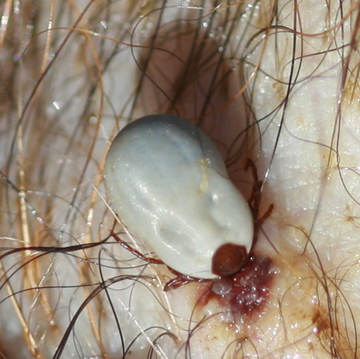
Adult ticks wait on shrubs or tall grass and attach to larger mammals such as people, deer, or pets. They also take several days to fully engorge (feed). A female fully engorged with a blood meal can be almost the size of a dime, appearing smooth and shiny. Mating takes place on the host, and when fully fed, the females drop off and lay eggs. The life cycle can be as short as three months, but typically lasts two years. American dog ticks can survive a very long time without feeding. This species can transmit the organism that causes Rocky Mountain Spotted Fever, which is rare in New England but more common farther south. The tick is most active from May through July in New Hampshire.


Stories in the press have confused many people about the relationship of this tick and Lyme disease. Despite the fact the spirochete (bacterium) that causes Lyme disease has been found in American dog ticks, tests prove that the tick can’t transmit the organism to its hosts. Therefore, it isn’t involved in the spread of Lyme disease.
The winter tick, Dermacentor albipictus, is similar in size and appearance to the American dog tick. Unlike that species, the winter tick isn’t active in the summer and it completes its entire development on one host. It is often found on moose, deer, or horses during the fall, winter or spring. It doesn’t commonly bite people, and does not transmit agents that cause disease in people. Eggs of this species hatch in the spring, but the larvae remain bunched together in a torpor all summer long. They don’t become active until cold weather returns in the fall. As with other ticks, they wait on leaf litter or low vegetation for a host to brush by. After attaching to a suitable host, this species remains on the animal, feeding and molting until it has fully grown. Then it drops off, and eggs are laid on the ground in the spring.

In New Hampshire winter ticks have been collected as far south as Durham, Nottingham, Wilton and Roxbury, but the species is more abundant farther north. Hunters or other people active in the woods in October and November occasionally sit on, or place a hand on the ground in a group of larvae waiting for a host. As many as 50 larvae have been found on a glove or pant leg after such an encounter. The larvae are brown, about the size of a pinhead. Sometimes moose are found in winter with large patches of bare skin, carrying thousands of winter ticks. Such heavy infestations sometimes kill the moose. Recent research in New Hampshire demonstrates that winter ticks are limiting the moose population, and mortality of calves is especially high. Winter ticks are found in lower numbers (not hundreds per animal) on deer. Adult winter ticks look like slightly elongated versions of the American dog tick.
The brown dog tick, Rhipicephalus sanguineus, is uncommon in New Hampshire, though it probably occurs throughout the state. This species is slightly smaller and slightly different in shape than the American dog tick. It is reddish-brown in color and lacks the mottling the Dermacentor species have. It has a life cycle very similar to other three-host ticks (like the American dog tick). It can be a problem in kennels and zoos, but rarely bites people. It has a strong tendency to crawl upwards and hides in cracks in kennel roofs or in ceilings or porches. In heated buildings, it can appear at any time of the year. It is unlikely this tick would be found anywhere but in or adjacent to kennels or houses where dogs are kept. This species can spread two diseases to dogs: canine ehrlichiosis and canine babesiosis.

The blacklegged tick, Ixodes scapularis, is our second most common species, and soon it may become our most common tick. Until 1993, northern specimens were considered a different species, called the deer tick (Ixodes dammini).
It looks similar to the tick species mentioned above, but is smaller and more rounded. It lacks the mottling of Dermacentor species. Adult males are very dark brown, almost black. Adult females are two-toned: dark chestnut brown on head, legs and scutum, and orange-red on the rear half of the body. Nymphs are about the size of a pinhead (1-2mm), and adults are just over 1/16” (2-3 mm) long. When fully engorged with a blood meal, an adult female blacklegged tick can swell to 3/8-inch (10 mm) long.
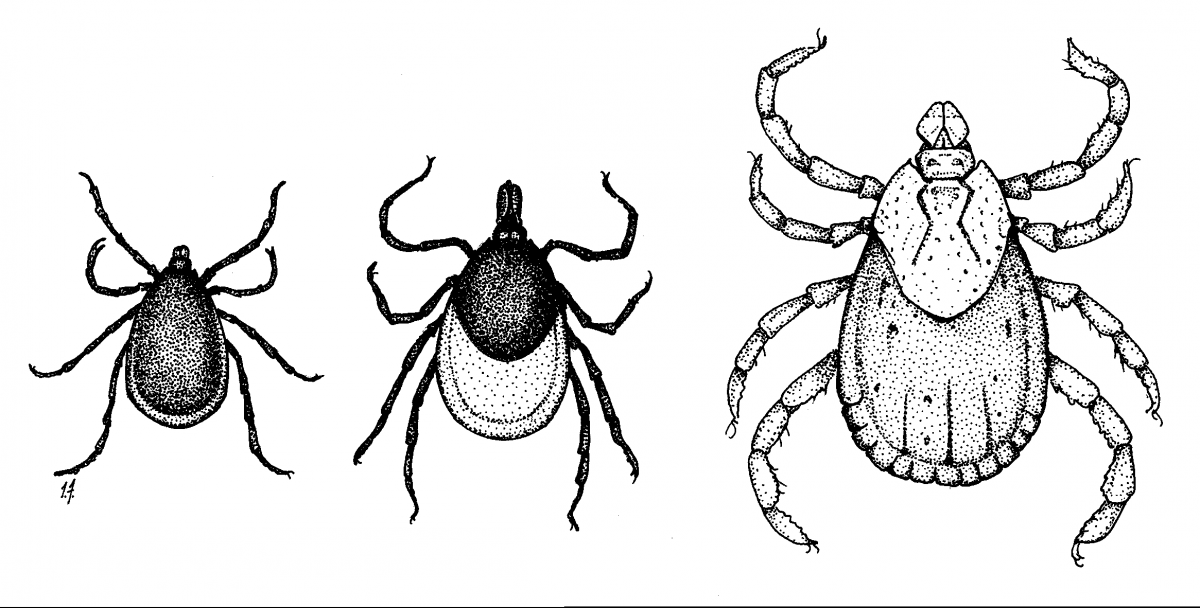
This species has received much attention because it is the vector of (transmits) the organism that causes Lyme disease. A 2007 study also found two additional pathogens in some N.H. blacklegged ticks: the pathogens that cause babesisis and anaplasmosis in people. Some New Hampshire specimens may carry Powassan virus.
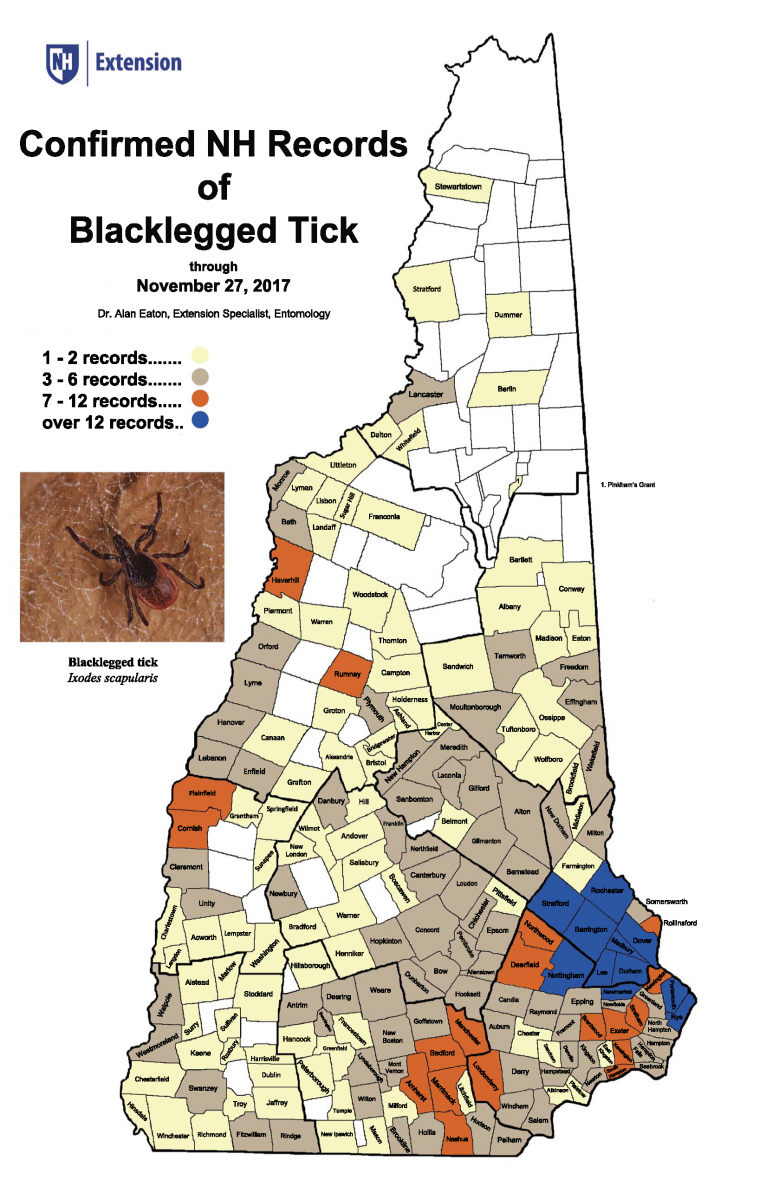
Blacklegged ticks occur in all ten counties, but are most abundant in the southeast. In 2007, about 85 percent of the population was found within 35 miles of the coast. In 2015, 67% of my data points are within 40 miles of the coast. In the western part of the state, blacklegged tick numbers are higher close to the Connecticut River, compared to farther away. The current data map is compiled from 1) samples submitted for identification, 2) examining deer and moose at hunter check stations, and 3) collecting ticks on vegetation with a tick drag (which is called “flagging”). The map still has some bias for locations close to the University of New Hampshire, since people close by are more likely to submit ticks than those farther away. The coastal-abundance pattern occurs in many other states, including Maine and Massachusetts. This tick now occurs in New Hampshire in much higher numbers than a few years ago. This could be from many factors, including increasing deer numbers, increasing human population, and creating more edge habitat by building houses in wooded areas.
The life history of the blacklegged tick is typical of other three-host ticks. The life cycle takes two years. Larvae are most commonly found on mice, other small mammals, and birds. Nymphs commonly bite these hosts, as well as medium-sized animals and people. Adult ticks most commonly attach to large animals, such as white-tailed deer. They are most active from early October to late-November, plus late March through May. Activity continues in mild winter weather (temperatures above 40F) when there is no snow cover. Nymphs are most active from May 15th through early or mid-July. This species will readily bite people. Scientists have shown that high populations of deer are necessary for this tick to be abundant. Observations in New Hampshire support this finding. In Massachusetts, the incidence of Lyme disease is strongly linked with high deer populations.

There are other New Hampshire ticks that are very similar to the blacklegged tick. Ixodes muris is a species that is commonly associated with mice and other small mammals (and their predators) and people. It is very similar to the blacklegged tick, especially in the nymph stage. Researchers in Maine proved that it can vector Lyme disease, but is a relatively inefficient vector, compared to blacklegged tick. They also reported that domestic animals bitten by this species sometimes show severe reactions (pain, swelling, lethargy, etc). In New Hampshire, I. muris records predominately are from Rockingham and Strafford counties.
Woodchuck tick, Ixodes cookei, is a species that occurs in every New Hampshire county. It is commonly found on a variety of small and medium sized mammals, as well as people. It is similar in size to the blacklegged tick, but under a microscope there are obvious differences. It is not involved in the spread of Lyme disease, but is a vector of a rare, serious human disease called Powassan encephalitis. A case of this disease was confirmed in Hillsborough County, in 2013. Ixodes banksi is another close relative of blacklegged tick. It is strongly associated with beavers and muskrats. Another relative is Ixodes marxi, which is strongly associated with squirrels.
The lone star tick, Amblyomma americanum rarely turns up in New Hampshire. It is unclear whether the specimens that are encountered actually overwintered here, or if they “hitchhiked” from farther south. Its reported range reaches to coastal Connecticut and Rhode Island. The adult females are red-brown, with a prominent white dot. The lone Star tick is the vector for Ehrlichia chaffeensis, the agent of human monocytic ehrlichiosis (HME), and Ehrlichia ewingii, which causes human and canine granulocytotropic ehrlichiosis. Lone star ticks cannot spread Lyme disease.
Although several other species of ticks live in New Hampshire, most people rarely encounter them.

Tick-Borne Diseases
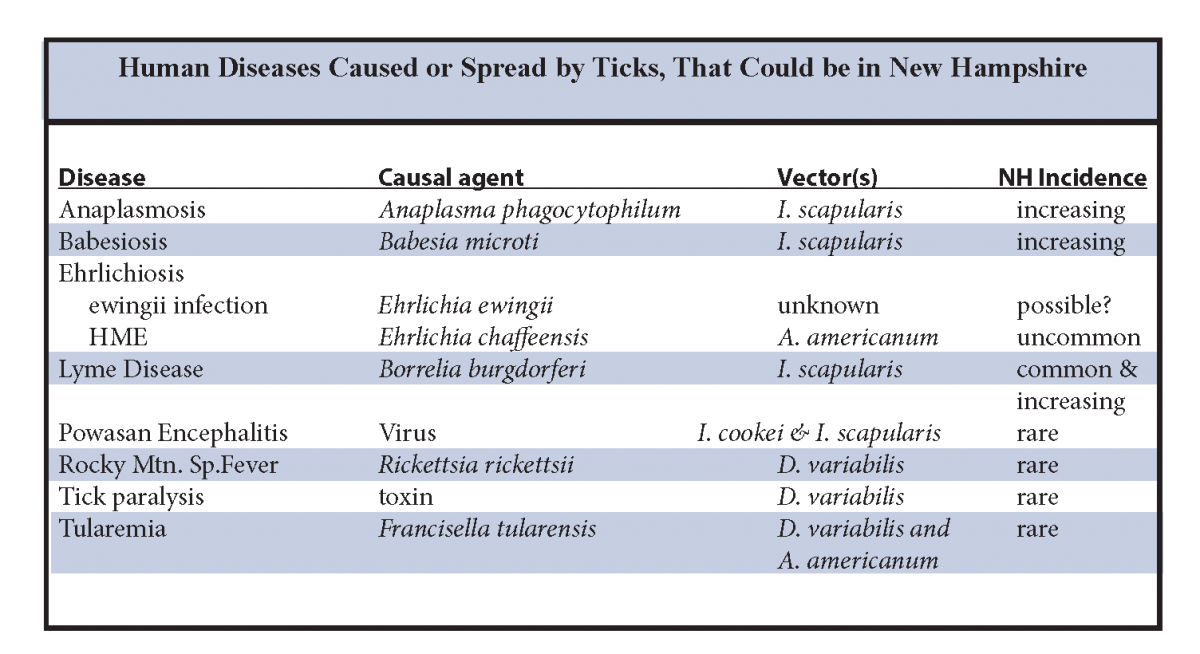
Ticks can spread several diseases, but except for Lyme disease, anaplasmosis and babesiosis, the incidence of such illnesses is rare in New Hampshire. Other illnesses include Rocky Mountain spotted fever, tularemia, tick paralysis, Powassan encephalitis, Colorado tick fever and ehrlichiosis.
Lyme disease is the most common vector-borne (transmitted by insects or ticks) disease in the U.S. It was first identified in the U.S. near Lyme, Connecticut, in the mid 1970s. It is caused by a spirochete, an elongated, corkscrew-shaped bacterium named Borrelia burgdorferi. In the latest (2014) data from the U.S. Centers for Disease Control and Prevention, New Hampshire ranks seventh in the nation in the number of Lyme Disease cases reported per 100,000 people. The rankings change slightly from year to year, and our state has ranked as high as first in recent years. In New Hampshire, most cases are reported from Rockingham, Hillsborough and Strafford Counties.
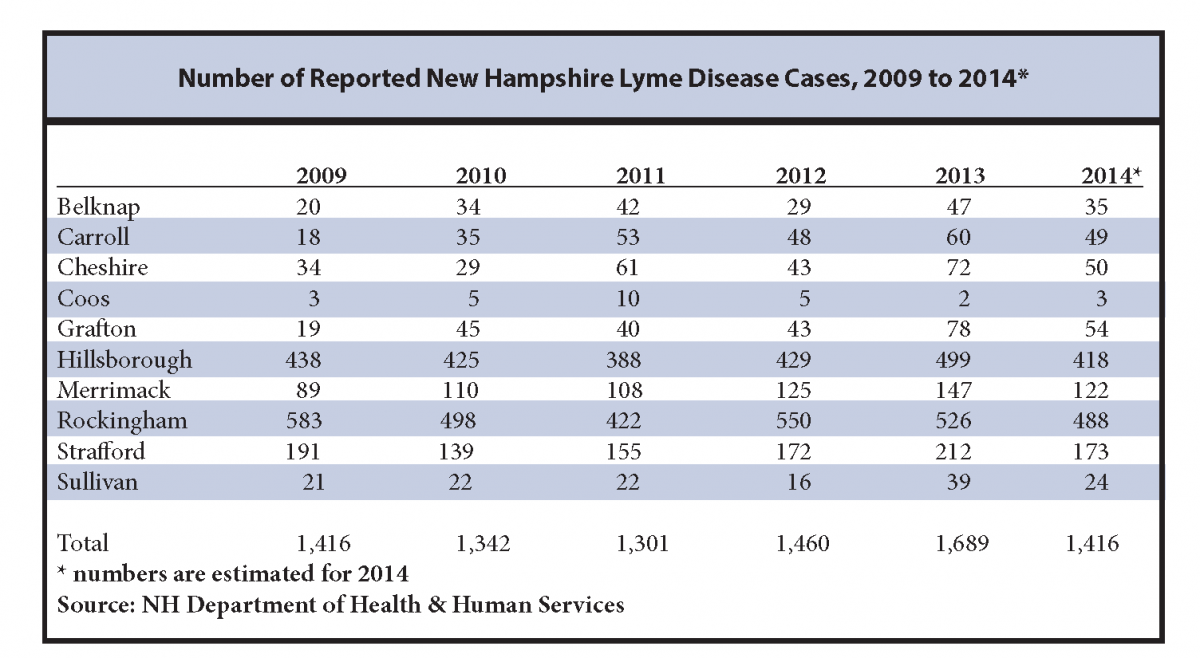
From 2007 to 2010, the N.H. Department of Health and Human Services sampled blacklegged ticks during fall months. More than 50 percent of the adult blacklegged ticks tested in Cheshire, Grafton, Hillsborough, Merrimack, Rockingham, Strafford, and Sullivan Counties were infected with the causative Lyme disease pathogen Borrelia burgdorferi. Between 20 and 50 percent were infected in Belknap and Carroll Counties. The tick numbers were too low in Coos County to estimate infection rate. Statewide, nearly 60% of adult blacklegged ticks were found to be infected with Borrelia burgdorferi.
In a followup study examining ticks collected during the fall and spring months of 2013 and 2014, infection with Borrelia burgdorferi was identified in more than 50% of adult blacklegged ticks collected in Belknap, Grafton, Hillsborough, Merrimack, Rockingham and Strafford Counties. Not enough ticks were collected in Carroll, Cheshire, Coos or Sullivan Counties to reliably estimate infection rates. Sampling from this time period showed that the statewide infection prevalence rate of adult blacklegged ticks remained close to 60% for Borrelia burgdorferi. Maps for both of these testing events may be found a on the NH Department of Health and Human Services web page.
The cycle of transmission begins with a blacklegged tick larva or nymph feeding on an infected reservoir host. In a reservoir host, after getting infected with the disease agent, the infective agent builds up to a relatively high level in the blood, but the animal doesn’t show ill effects. Ticks feeding on infected reservoir hosts pick up the spirochete along with their blood meal, so reservoir hosts serve as amplifiers for the pathogen. The white-footed mouse is the major reservoir host for Lyme disease in New Hampshire. The feeding tick picks up the bacteria along with its blood meal. After feeding, the tick digests its meal and transforms to the next life stage. This takes weeks or months. When the tick attaches to another host and begins feeding again, the bacteria multiply in the tick’s gut. Some of them penetrate the gut wall and travel to the salivary glands. As the tick continues to feed, it injects some bacteria into the host, along with the tick’s salivary secretions. Infected adult blacklegged ticks require more than 24 hours of feeding to transmit the bacteria. Nymphs may transmit the disease organisms to their host in 24 hours of feeding, or possibly less.
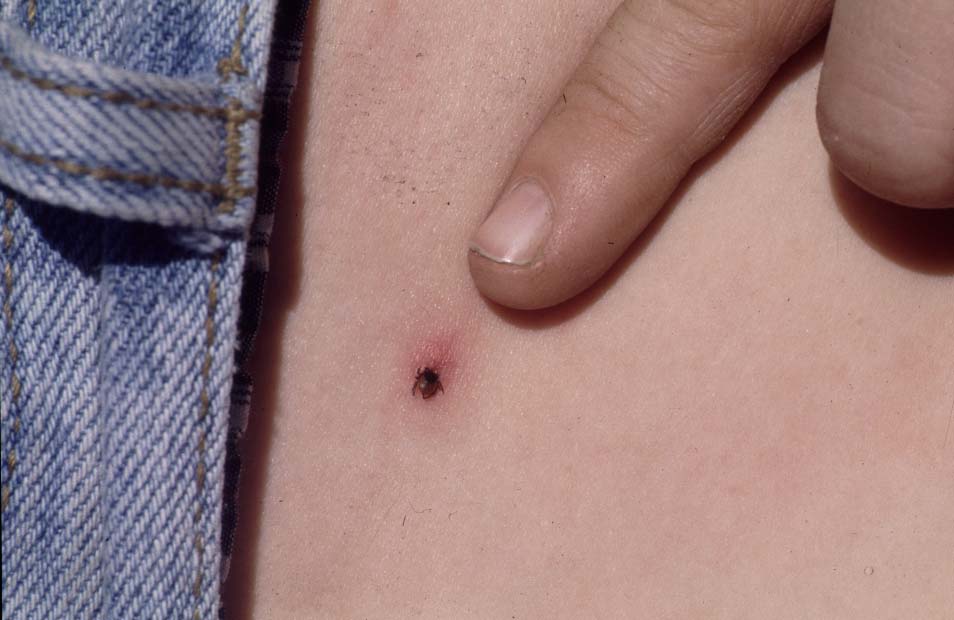
Symptoms of Lyme disease in people frequently (70-80% of those infected) begin with a characteristic red zone (rash) around the site of the bite. It usually appears three to 30 days after being bitten by an infected tick, and it slowly expands in size, then fades. Don’t confuse this red zone with the red spot that appears within hours where you’ve removed a biting tick. The Lyme disease rash is often ring-shaped and may be warm to the touch. The photo shows it as fairly dark, but it can be much fainter. Fatigue, fever, headaches, stiffness and pain in muscles and joints often occur. They can appear from a few days to weeks after infection. Do not confuse a red mark that forms during biting with the LD rash, which appears some time after the tick has been removed.
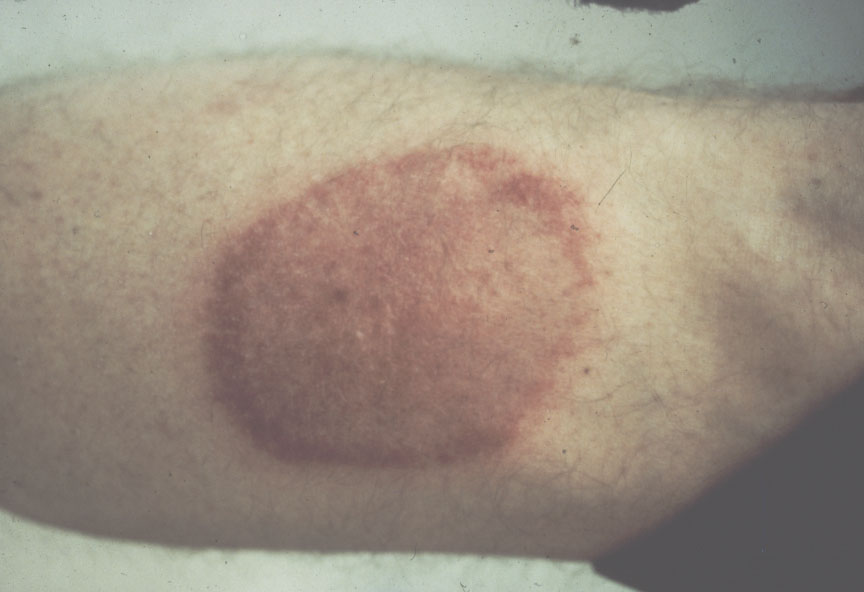
If Lyme disease is left untreated, dizziness, irregular heartbeat, arthritis, and nervous system disorders as well as joint pain and swelling can follow days to months after the bite from an infected tick. Arthritis, joint pain and swelling most commonly are seen in knees or other large joints.
Most cases of Lyme disease are contracted in late May through mid-July, when the nymphs are active. In people, most cases are transmitted by nymphs, because they are very small and easily overlooked. Also, nymphs can transmit the organism faster than adult ticks. Treatment is most successful in the early stages, and antibiotics are used. For a while there was a human vaccine for Lyme disease, first approved by the FDA in December 1998. It is no longer available. Dogs, and to a lesser extent, horses and cattle also suffer joint disorders caused by the Lyme disease bacterium.
Ehrlichiosis is the name for several diseases of animals and humans. Ehrlichia chaffeensis is the agent of human monocytic ehrlichiosis (HME). Ehrlichia ewingii causes human and canine granulocytotropic ehrlichiosis. Victims usually report flu-like symptoms (headache, fever, muscle aches, fatigue) and sometimes gastro-intestinal symptoms or rash. Symptoms typically appear five to ten days after being bitten by an infected tick. The lone star tick (rarely encountered in N.H.) is the primary vector. Most cases appear in the southern, eastern and south-central states. Between 2010 and 2014, 28 cases of human ehrlichiosis were reported in New Hampshire. These were most likely associated with travel to areas where the lone star tick is found, rather than infection from ticks found in New Hampshire. Forms of ehrlichiosis also occur in horses and dogs.
Anaplasmosis. Human granulocytotropic anaplasmosis is a new name for a relatively new tick-borne disease formerly called HGE (human granulocytic ehrlichiosis). The number of reported cases has been rising for several years, with the highest incidence in people over 60. In 2010, the highest incidence was reported from Minnesota, Wisconsin, New York, New Jersey, Delaware, Connecticut, Rhode Island, Vermont, New Hampshire and Maine. From 2010 through 2014, 320 cases of Anaplasmosis were reported in New Hampshire. The number of cases increased each year.
The causal organism is a bacterium called Anaplasma phagocytophilum. In the eastern United States, blacklegged tick is the vector. Deer and wild rodents are thought to be the reservoirs for this disease. A 2007 study of adult blacklegged ticks from New Hampshire confirmed the presence of Anaplasma-infected ticks in Hillsborough and Rockingham Counties.
People with anaplasmosis commonly report flu-like symptoms (headaches, chills, fever, muscle aches), with the onset of symptoms one to two weeks after being bitten. Physicians treat the disease with antibiotics.
Babesiosis is a human disease caused by a protozoan (most commonly Babesia microti, although other species are known to cause disease) that attacks red blood cells. The microorganism is related to malaria parasites, and there are similarities in the two diseases. Babesiosis is associated with voles, chipmunks, mice and shrews. The white-footed mouse is the primary reservoir host. Human cases have been increasing in the northeast since its recognition in the 1970s on Nantucket, Block Island, and parts of nearby states. The blacklegged tick is the main vector. Most human cases occur during summer, when blacklegged tick nymphs are active, but adults can also spread the disease.
Symptoms range from asymptomatic to life-threatening, and include fever, fatigue, chills, sweats, headache, and more. Severe symptoms are more likely in people who are immunosuppressed, have had their spleen removed, and/ or are elderly. Onset of symptoms is extremely variable after the tick bite, ranging from weeks to months. From 2010 to 2014, 107 cases of human babesiosis were reported in New Hampshire. The number of cases increased each year.
In a 2007 study for the NH Department of Health & Human Services, adult blacklegged ticks were collected across New Hampshire and analyzed. They detected low to moderate prevalence of Babesia microti in Strafford, Rockingham, Merrimack, Hillsborough and Carroll Counties.
Rocky Mountain Spotted Fever. This disease is caused by a bacterium called Rickettsia rickettsii. Until about 1930, it was thought to occur only in the Rocky Mountain region, hence its name. Today there are far more cases reported in the eastern states, especially in the South-Atlantic and West-Central states. North Carolina and Oklahoma have the highest number of cases. From 1997 to 2002, one case of Rocky Mountain Spotted Fever in a person was reported in New Hampshire. During that period, Connecticut had five cases; Massachusetts had 13, Rhode Island had nine, and there were none from Vermont or Maine. Between 2010 and 2014, there were 12 cases reported from New Hampshire. There is no evidence of local transmission of this disease in New Hampshire at this time.
The disease usually appears in late spring, summer or early fall. American dog tick is the principal vector, but brown dog tick has also been implicated.
Two-thirds of the cases occur in children under age 15. Symptoms usually appear two to 10 days after being bitten by an infected tick. Headache, backache and fever are common symptoms. A spreading, spot-like rash usually develops, often beginning on wrists and ankles. Prompt diagnosis and treatment with antibiotics are important. Fifteen to 20 percent of untreated cases are fatal. The disease is treated with antibiotics.
Powassan Encephalitis. The causal agent of this very rare, sometimes fatal disease is a virus (a flavavirus). Recent cases appeared in nine states, with the highest U.S. numbers in Minnesota, New York and Wisconsin. It was first described from Powassan, Ontario in 1958. The first U.S. case was 1970, in New Jersey. Ixodes cookei and blacklegged tick are the principal vectors. The virus has also been found in Ixodes marxi, but that species hasn’t been proven as a vector. Encephalitis is a disease that causes swelling of the brain. As with Eastern equine encephalitis, some survivors have long-term neurological problems. Recent screening for West Nile virus has increased the number of cases discovered. The first case in New Hampshire was found in Hillsborough County, in the summer of 2013. As with other arboviral infections, such as Eastern equine encephalitis, there is no specific treatment for Powassan virus encephalitis, just supportive care.
Tularemia. “Rabbit fever” is caused by the bacterium Francisella tularensis. The disease can be contracted from skinning and cleaning infected rabbits or from being bitten by infected ticks. Tularemia occurs throughout the United States, but is rare in New Hampshire. Most U.S. cases occur in Missouri, Arkansas and Oklahoma. In the East, most cases occur in the fall and winter and are presumed to be associated with hunting rabbits or other small animals. Symptoms depend on the route of infection. When acquired by a tick bite, an ulcer often forms at the site of the bite. Fever is a common symptom. Swelling of nearby lymph nodes sometimes occurs. Antibiotics can be used to treat the disease. The American dog tick is the vector species that occurs in New Hampshire. Lone star tick (very rare in N.H.) can also spread the disease. Several cases are known from Martha’s Vineyard, Massachusetts.
Tick Paralysis is caused by toxic substances in the secretions of some feeding ticks. In people, it occurs most frequently in children under the age of seven. Young girls are common victims (probably because it is difficult to detect ticks in long hair). The most frequent site of biting that causes “paralysis” in people is the back of the neck, close to the hair line. Victims have difficulty moving or controlling arms or legs. When you discover and remove the feeding tick, these symptoms disappear within an hour or two. In the United States, it is more frequently seen in the Southeast and Northwest. The American dog tick can cause tick paralysis. The condition is also reported in dogs.
Safe Removal of Ticks
Since tick bites are painless, ticks are often discovered after they have begun to feed. Removal is fairly easy, provided it is done correctly. We recommend using tweezers to grasp the tick, rather than using bare fingers. Using bare fingers may contaminate them with a disease-causing organism.
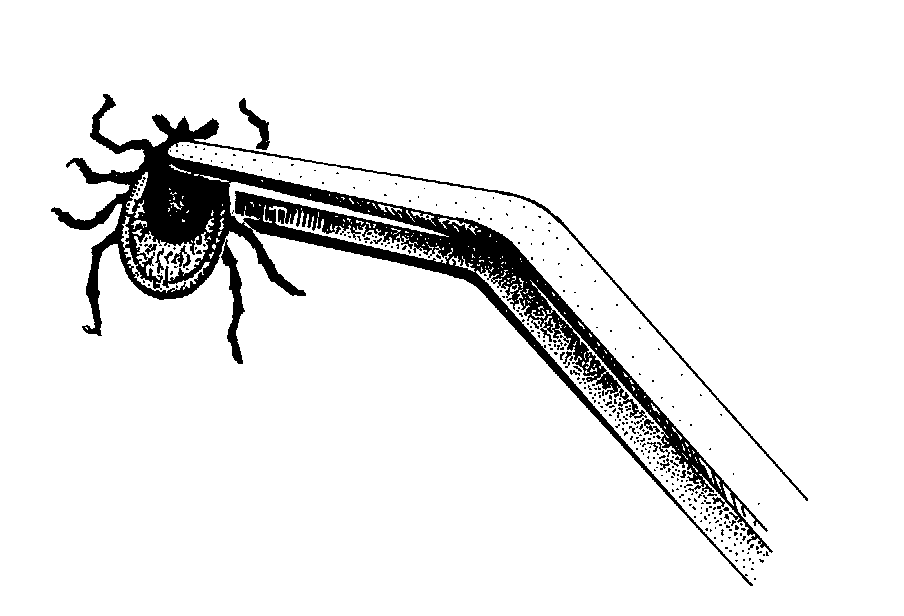
Also, it is easier to get a firm grip of the head with tweezers. Firmly grasp the tick as close to its head as possible, and pull gently, using slow, steady pressure. DO NOT yank it or pull it sideways, since this could cause its head to break off inside the wound. It might take as long as a minute or two for removal. Some people find it easier to use a plastic tick spoon, called “Ticked Off ”. You slide the spoon under the attached tick, fitting its mouthparts into the v-shaped notch. Then hold the body of the tick down with your thumb, and gently roll the handle of the spoon down, using leverage to pull the tick out. Be careful to fit the mouthparts into the smallest part of the notch, and do this as close to the skin as possible.

Touching a hot match to an embedded tick, or covering it with Vaseline or other substances aren’t recommended. They do not help to remove the tick, and we worry that they might increase the likelihood of the tick regurgitating into the host (possibly injecting disease agents). Check to be sure the head comes out, rather than breaking off. The photographs should help determine if all of the head has come out. It may be wise to apply an antiseptic to the wound after removing the tick.
Tick Testing
New Hampshire homeowners, gardeners, hikers, hunters, landscapers and anyone else who works or plays outdoors can now have ticks identified and tested for dangerous tick-borne illnesses, like Lyme disease, anaplasmosis, babesiosis and Powassan virus.
How to Submit a Tick for Testing
-
Place tick (dead or alive) in a sealed plastic bag
-
Write order number on bag
-
Send to TickReportTM - Laboratory of Medical Zoology, 101 Fernald Hall, University of Massachusetts, 270 Stockbridge Rd, Amherst, MA 01003
-
Receive e-mail results in 3 business days
*Please note that you were referred by UNH Extension.
UNH Extension has teamed up with UMass's TickReportTM to provide this tick identification and testing service.
Protecting Yourself From Tick Bite
The Public Health Services division of NH Department of Health and Human Services released a comprehensive report on preventing tick-borne diseases. The most obvious way to avoid contact with ticks is to stay away from tall grass and brushy areas that are prime tick habitat. May through August are prime months for the American dog tick. April through July, and October through mid-November are periods when blacklegged tick nymphs or adults are most active. If you do spend time in tick-infested areas, wear proper clothing. Wear good shoes (no sandals or bare feet) and long pants tucked into your socks. People who work in brush might prefer to use gaiters. They are stretchy material that fit over the laces and tops of boots, and can hold tucked pantlegs securely. A long sleeved shirt with snug collar and cuffs will also offer protection, if it is tucked in at the waist. Dressing this way helps keep ticks you do encounter on the outside of your clothing, where they may be spotted or brushed off. Light colored pants and shirt allow you to easily spot crawling ticks.
There are also several forms of tick-proof or tick-resistant clothing. Some are made of tightly woven, slick material to which ticks can’t easily attach. “Tick Chaps” is one example. Others are made of fine mesh netting through which adult ticks can’t pass, like “Bug Baffler.” Wearing tall (16 inch) rubber boots can reduce the number of ticks that get onto you. The smooth rubber surface is difficult for ticks to grab onto.

You can treat clothing with tick repellent for added protection (see below). There are several effective active ingredients. Socks, ankles, legs and pant legs are the best places to treat. Always read and follow label directions, when using repellents.
Pressurized spray products containing the insecticide permethrin are registered for protection against ticks. They are sprayed on clothing, and repel and/or kill ticks that attach themselves to the clothing. Such products should never be applied to skin. After spraying on your clothing, allow it to dry an hour or more before you put it on. Permethrin adheres very well to cotton, and is long lasting (often through numerous washings).
If you have been in tick-infested fields or woods, monitor yourself, your children, and pets every day during tick season. Undress to check for ticks. For many people, bedtime is the most convenient time to do this.
A full length mirror or family member can help you see ticks on your back or other difficult to see areas. Don’t neglect to check your head, especially if you have long hair. Ticks tend to crawl upward, and if they can’t get inside your clothing, they will end up on your head or neck. If you find a tick that has already begun to feed, carefully remove it as described previously. If you are concerned it might be a type that transmits disease, place it in a container and take it to UNH Cooperative Extension or the State Entomologist for identification (addresses at end). Be sure to record the date and location of the bites. If possible, record the date and where (town) you probably picked up the tick. This can simplify its identification.
If a tick has been biting less than 24 hours, your chance of getting Lyme disease from that bite is extremely small, possibly zero. It is possible to get Anaplasmosis from a shorter duration bite. But just to be safe, monitor your health closely after a tick bite and be alert for any signs and symptoms of tick-borne illness. If symptoms show up, consult your physician for advice. Be sure to give your doctor details about where and when you were bitten, and any symptoms. If your pet has joint disorders, you may wish to see your veterinarian for advice.
Repellents
The most effective repellents for ticks contain a material called n, n-diethyl-m-toluamide or “Deet.” Check the label of your insect repellent, and see if it is contains this material. Socks, ankles, legs and pant legs are the best places to treat, if ticks are the target. When applying to the skin, use Deet sparingly, with care. A small segment of the population may be sensitive to it. Be careful not to get it in eyes or mucous membranes, and be especially cautious of its use on young children. It should not be used on infants. Deet has some other drawbacks. It can dissolve some plastics and some finishes, and it has a greasy feel.
Picaridin is a repellent that works very well on mosquitoes, and does fairly well against ticks. It has been available in New Hampshire since about 2006. For people who are concerned about sensitivity to deet, this is a good alternative. Some NH-registered picaridin repellents list ticks on the label, and others do not. This may reflect differences in concentration --- the ones that list ticks usually have a higher percentage of picaridin.
IR3535 [ethyl butyl acetyl aminoproprionate] has several chemical names. The chemical was designed in the early 1970’s, and has been available in Europe since the mid-1970’s. Tests show that it works moderately well on mosquitoes, and fairly well on blacklegged tick. At least three manufacturers (Sawyer, Chattem, and Avon) make products that combine sunblock and insect repellent, contain this chemical, and are registered for use in NH. The Chattem (“Bullfrog Mosquito Coast”) and Sawyer products typically have 20% IR3535 and are registered for mosquitoes. The Avon products have lower % active ingredients, and are registered for “biting midges, black flies, deer ticks, gnats, mosquitoes, no see-ums, and sandflies”.
A repellent recently registered with EPA, 2-undecanone, is derived from wild tomato plants. Some chemical registries refer to the same compound as methyl nonyl ketone. It worked as well as or better than deet in preliminary published tests on American dog tick. BioUD is a trade name for products with this active ingredient. It was last registered in New Hampshire in 2010, but has not been re-registered here. Other tick repellents reported in scientific journals include A13-37220 and tansy essential oil. Perhaps these will eventually appear in commercial tick repellents.
Amitraz and permethrin are two pesticides for ticks that show what is sometimes called repellency. Rather than being true repellents, they seem to create irritation and toxicity symptoms in ticks, which cause ticks to drop off and prevents them from attaching. Tick control products containing fipronil can also prevent tick attachment, which some people interpret as “repellency”.

Reducing the Threat of Ticks on Your Property
The greatest natural mortality factor for ticks is drying out. There are a number of steps you can take on your property to make vegetation and leaf litter dry out faster, and be less favorable for ticks. One is to keep the lawn mowed, and keep a mowed strip between play areas and thick brush. Removing dense brush might also be helpful in some situations. A second technique is to reduce human contact with the tall grass or thick brush that holds ticks. This could be by widening paths through the woods, moving play equipment away from the woods edge, or mowing the edges of paths. You might consider using black plastic landscape netting or other fencing to limit people from walking into thick vegetation along paths. This might be effective for property open to the public, like parks. (Ticks often occur in high numbers right next to roads, paths, and game trails.) Spraying is another option.
Spraying with Pesticides
There are many products that can be sprayed to kill ticks. Most are intended for outdoor use. Indoor treatment might be helpful to control brown dog tick. Some pesticides are registered for use on pets, as sprays, topical spot treatments, or collars. The pesticide label will specifically indicate where and how these can be used. For controlling ticks outdoors, an early June insecticide spray to the leaf litter can be effective to control the nymphs of blacklegged ticks in your yard. The perimeter of yards, shaded perennial beds, along woods trails, and stone walls are important target areas. Lawns are not important areas to spray (too dry). A sprayer that has enough pressure to turn over leaves and vegetation, and reach into crevices is most effective. In many cases, this means hiring a professional pesticide applicator. Treatment in October can be effective on blacklegged tick adults if the lower three feet of brush and shrubs are targeted. To control American dog ticks and nymphs of blacklegged tick, a Spring (May 15) treatment can be effective. As with any pesticide purchase, it is essential that you first read the pesticide label to be certain that the one you intend to buy is registered for the intended use. The target pest (ticks) must be in the label instructions, along with the site. Application of any pesticide “in a manner inconsistent with its labeling” is a violation of both state and federal laws. For those people with restricted use pesticide licenses, there are many more options. Chemical choices for outdoor spraying include carbaryl, synthetic pyrethroids, and some products with essential oils.
Indoor treatment might be helpful to control brown dog tick. That species has a strong tendency to crawl upwards and lay eggs in crevices of kennel roofs or ceilings. The immatures then move downwards and hide in cracks and crevices of walls, floors, windows, etc.
Some products contain pesticides that have relatively low risk of causing problems, thus are available to anyone (“general use materials”). Others have a greater risk of causing problems if users do not carefully follow directions. These (restricted use products) are available only to licensed pesticide applicators or professional pest control personnel.
Pesticides Used for Tick Control
Carbamates - Carbaryl (“Sevin”) is a broad spectrum insecticide which controls ticks well. Broad-spectrum means that it kills a very wide range of insects, including many beneficial species. Outdoors, the sunlight, oxygen and moisture work to break down the chemical relatively quickly. Residues typically kill pest insects for 5 to 10 days after spraying. Carbaryl is incorporated into some tick collars, plus some sprays sold for use around homes. It is very toxic to bees and many other beneficial insects, and moderately toxic to mammals.
Propoxur is another carbamate chemical that controls fewer kinds of insects (“narrower spectrum”). It is in some tick collars, and is highly toxic to mammals, so is used at low concentrations.
Formamidines - Amitraz is the only current tick-registered chemical in this group. It is in some tick collars for pets. It is a somewhat narrow spectrum material, effective on mites, ticks, and some insects. It has slight toxicity to people.
Insect Growth Regulators - These are relatively new chemicals. They interfere with the hormones that control insect development, which are quite different from human hormones. Immature stages of insects (and some mites and ticks) are vulnerable, but adults are not. These chemicals generally have very low risk of mammalian toxicity. Pyriproxifen and s-methoprene are in this group, and are in some flea & tick collars, and some indoor treatments. Both have low toxicity to people and other mammals. Methoprene is not very effective on ticks, but does kill fleas.
Organo-phosphates - Formerly there were several insecticides in this group that were widely used for tick control, including chlorpyrifos (Dursban) and Diazinon. The Food Quality Protection Act (1996) initiated a review of the safety and toxicity of these materials, and neither is available for this purpose today.
Rabon (tetrachlorvinphos) is a relatively long-lasting organo-phosphate in some tick collars and some sprays. It has moderately low toxicity to humans, and has been used as a livestock feed additive to control flies.
Phenylpyrazoles - Fipronil is used in products to protect pets from ticks and fleas. It dissolves in the oils on the skin, spreads over the body, and collects in sebaceous glands, where it is slowly released over several weeks. It is slow acting, and is highly toxic to people. “Frontline” is a product with fipronil.
Pyrethrins - Pyrethrum is a mixture of many “pyrethrins”, which are chemicals produced by a flowering plant, Chrysanthemum cinerariaefolium. Pyrethrins have been used for many years to control insects. They have rapid knock-down effects on most insects, but some species recover from this. For this reason, pyrethrins are often mixed with other insecticides or a synergist. The most common synergist is piperonyl butoxide, sometimes abbreviated PBO. Another is n-octyl bicycloheptene dicarboximide. The synergist greatly enhances the effectiveness of pyrethrins. Pyrethrins are rapidly broken down by sunlight, moisture and oxygen, often within hours of application. They are generally low in toxicity to mammals, which is one reason they are often labeled for indoor use and on pets. They are not good choices for treating outdoors, because they have such short lived action.
Synthetic Pyrethroids - Pyrethroids are artificial chemicals that were invented after chemists studied pyrethrins. Pyrethroids are very broad spectrum insecticides with long residual action. They are much more slowly broken down than pyrethrins, so the residues sometimes kill insects for weeks after application. Common examples for tick control include bifenthrin, cyfluthrin, cypermethrin, cyphenothrin, deltamethrin, lambda-cyhalothrin, permethrin, and phenothrin. Many products with these chemicals are registered for spraying outdoors. Deltamethrin is used in some tick collars. It has fairly low toxicity to mammals, and fairly long residual action. Permethrin is used for some clothing spray-on treatments, and sprays in and around homes. It has low toxicity to most mammals, has low volatility, low water solubility, and is nearly odorless. It has long residual action. Phenothrin and Cyphenothrin are in some pet topical spot treatments and shampoos. They have low toxicity to mammals. Most of the other chemicals are used outdoors (or indoors by trained pest control people).
“Soft” Pesticides - Many people want to use a “green” or “soft” pesticide. Some are not very effective, yet are allowed on the market. The Environmental Protection Agency de-regulated “natural” products on the GRAS list (Generally Regarded As Safe) in May 1996. Since then, manufacturers of GRAS list products do not have to prove that they are effective, to get EPA registration as pesticides. For all other chemicals, manufacturers must prove that they work to get them registered for use in the US. There is one group of “soft” materials that holds promise. Several products incorporate essential plant oils and mineral oil. One such product performed relatively well in recent pilot tests on blacklegged ticks --- Eco Exempt IC2, now called Essentria IC3 [from Envincio LLC]. The largest active component [rosemary oil] is potentially toxic if ingested, but specific toxicity information on GRAS list products is hard to find. Another test published in November 2015 was on a garlic juice-based product. With multiple applications, it controlled nymphs of blacklegged tick relatively well, for short-term control. Testing of new products goes on continuously, so we may find still others in the future. Favorable testing results for one reached me just as this publication was being formatted for posting (March 2016). It is Met52, [from a company called Novozymes Biologicals, Inc.] an insecticide/acaricide with a fungus (Metarhizium anisopliae) as the active ingredient.
Soap-based insecticides might kill ticks, but they have disadvantages. They work by contact action, so the tick has to be directly hit by the spray. They don’t leave residues that kill. No soap-based insecticides that I can find have ticks listed on the label, which means you couldn’t legally use them to control ticks. The pesticide label is the law --- you must follow it.
Pesticides Aimed at Ticks on Small Wild Mammals
One way to reduce the threat of ticks around your home is to aim control chemicals at ticks on small mammals living in the vicinity. Two products have attempted this, and both ran into problems. One example is “Damminix tick tubes”. They are cardboard tubes filled with pesticidetreated cotton. The pesticide (permethrin) is very long-lasting, and effective on ticks. The idea is to spread these around the property, in places where mice and chipmunks will find it, and take the cotton as nesting material. Then, ticks feeding on them and dropping off in the nest would die. Most field trials with the product had disappointing results, but it is still available for sale in NH.
A newer product is a bait station available only through a contract with a licensed pest control company. It lures chipmunks and mice to feed on bait blocks, and in the process, get wiped with fipronil to control the ticks that attack them. I do not know how effective this strategy is, but the stations are called “tick boxes”. As this is being revised in December 2015, at least two pest control companies offer contracts with this product. Eco-Tech (in Eliot, ME) serves the seacoast of NH, while Atlantic Pest Solutions (Kennebunkport, ME) serves the entire state.

Protecting Pets
Your veterinarian can suggest materials to protect pets from ticks. Options include sprays, dips, shampoos, powders, collars, and topical spot treatments. Some can control ticks on dogs and cats for up to a month. Others work for a very short time. Shampoos can kill ticks on the animal, but have very short residual killing effect, if any. Fipronil topical spot treatment is absorbed by the body and gets concentrated in sebaceous glands (at the base of hairs) and their secretions. One treatment can kill ticks for weeks. Some methoprene (primarily acts on fleas), phenothrin, permethrin, and pyriproxifen products are applied as topical spot treatments too, and can last a long time. Tick collars usually contain the pesticides amitraz, deltamethrin, naled, propoxur (Baygon), or tetrachlorvinfos (Rabon) which are slowly released over time. Collars control ticks for a fairly long period of time. Some of them work by emitting toxic vapors. Others work by having the pesticide absorbed by the animal, and translocated throughout the body. Tick powders, shampoos and dips provide short term removal of ticks on an animal, rather than protect it for a long time. Usually they contain methoprene, permethrin, pryriproxifen, tetrachlorvinfos or pyrethrins plus synergists like piperonyl butoxide or n-octyl bicycloheptene dicarboximide.
Dog owners in areas with Lyme disease risk may wish to consult their veterinarian about vaccination, which is an option for some situations. Vaccination will not protect the animal from other tick-borne diseases. One obvious approach to protect pets is to regularly check for ticks, and remove them. This can be difficult, since small ticks are hidden by dense fur. Well engorged ticks are easier to find, but they have already had a chance to feed, possibly spreading disease to your pet.
Help and Information Sources
New Hampshire Division of Health and Human Services has Lyme Disease and other tick-borne disease information and maps.
The US Centers for Disease Control and Prevention has fact sheets, maps and information on many diseases.
New Hampshire Tickborne Disease Prevention Plan
New Hampshire Tick-borne Disease Bulletin
Alan Eaton’s 6-minute video on protecting yourself from tick bites
Tick Identification
1) The State Entomologist identifies ticks. New Hampshire Department of Agriculture, Markets & Food State Lab Building, 29 Hazen Drive, Concord, NH 03301.
2) UNH Cooperative Extension Insect Identification Center. G28 Spaulding Hall, 38 Academic Way, Durham, NH 03824. There is a $5 fee per specimen.
3) TickReportTM - For Pathogen Testing. This partnership between UNH Cooperative Extension and University of Massachusetts provides a resource for NH residents to send in and get ticks tested for disease organisms. Prices range from $50-$200.
This publication or parts thereof may be reproduced and distributed, provided that credit is given to the author and UNH Cooperative Extension as the source. Where trade names are mentioned, no discrimination is intended and no endorsement is implied. Pesticide registrations change frequently. For the latest information on registration of a pesticide in New Hampshire, contact the Pesticide Control Division of the NH Dept. of Agriculture at 603- 271-3550 or visit their website.
Acknowledgments
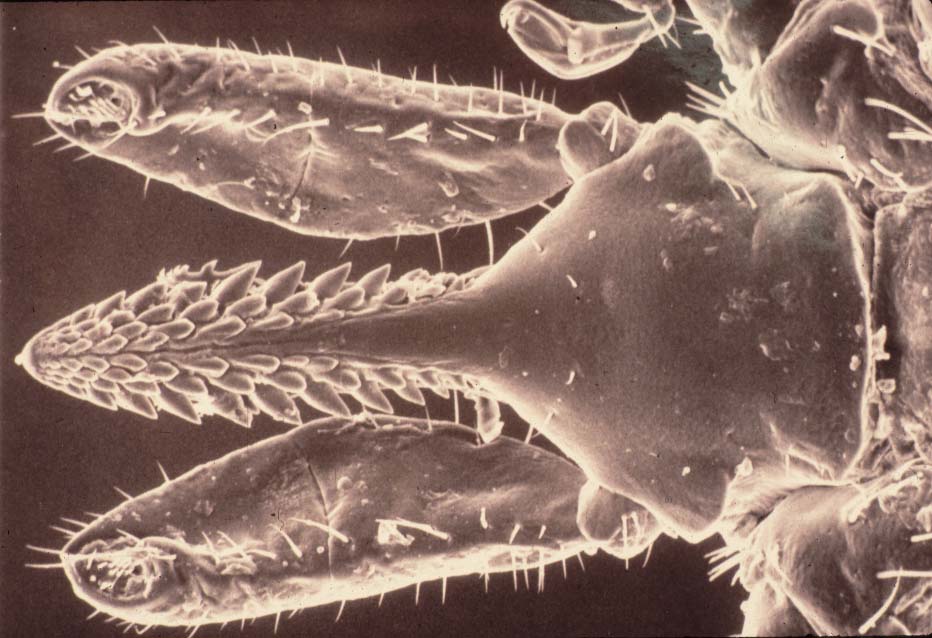
Dozens of people volunteered their time to assist with my three deer surveys, which provided many of the site records for black-legged tick. Thank you to all who helped make that effort work. Nancy Cherim, UNH Instrumentation Center, took the scanning electron microscope photo of blacklegged tick mouthparts. Pfizer provided the photo of ECM (rash). Faye Cragin took the photo of a repellant bottle label. Lise Laurin took the photo of a Lyme disease rash. All other photos are by Alan Eaton. Tess Feltes made the black & white drawings of blacklegged and American dog tick, plus the tick being removed with tweezers.
Thank you to Dr. Abigail Mathewson, NH Department of Health and Human Services, for reviewing the manuscript and making helpful suggestions. Suzanne Hebert did the layout and posting. William M. Samuel, University of Alberta (ret.) provided helpful corrections on winter tick biology.
Partial support for the recent revisions came from an Extension IPM Implementation grant from the National Institute for Food and Agriculture
Download the Resource for the complete fact sheet and a printable version.
If you liked this,

Get the best home, yard and garden advice delivered to your inbox
